Patients Information for Total Hip Replacement
Anatomy
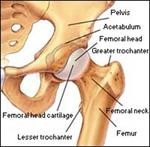
The hip is a ball and socket joint where the head of the femur sits in the cup-like acetabulum. A smooth cushion of articular cartilage covers the end of both these bones. The thick muscles of the buttock at the back, and the muscles of the thigh at the front surround the hip.
Healthy articular cartilage absorbs stress and allows the bones to glide across each other smoothly, allowing pain free movement and activities. The cartilage is kept slippery by joint fluid (synovial fluid) made by the joint lining (synovial membrane). The fluid is contained in a soft tissue enclosure around the hip called the joint capsule. The ligaments and strong muscles surrounding the hip give the hip power and stability.
What is Rheumatoid Arthritis (RA)
This is an inflammatory joint disease that can affect many joints within the body. It can cause swelling and heat in the joint lining. As the disease progresses it destroys the articular cartilage and eventually the bone itself is affected. Joints are usually painful, hot, swollen and stiff.
What is Hip Osteoarthritis (OA)
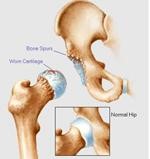
This is a degenerative disease and is often referred to as wear and tear arthritis. Years of normal use can cause the cartilage to crack and wear away and it is not able to heal itself. As the ends of the bones rub against each other, they become rough and pitted and eventually the cartilage may wear away altogether. Small outgrowths of bone spurs, called osteophytes, may form around the joint. At first the hip may be stiff, but as the bones begin to rub together you are more likely to feel increasing pain.
The onset of osteoarthritis can occur from previous injury to the hip. Cartilage injuries, infection or bleeding within the joint can also damage the joint surface of the hip. According to the World Health Organisation osteoarthritis affects half of the world’s population over the age of 65. The causes are not well understood. Ageing and genetic factors are among the major causes associated with OA
What are the alternatives to Hip Replacement
Not everyone wishes to have, or requires, a hip replacement when they have damaged their articular cartilage. Some people will have different pain tolerances and others may not wish to undertake the risks this surgery carries. Others choose to accept and live with the pain they have.
Alternatives to Hip surgery include:
- Regular pain medication.
- Using walking aids to relieve any stress on the joint.
- Weight loss to reduce the stress on the joint.
- Exercises to maintain joint movement, muscle strength and help pain relief.
- Adaptations and modifications to furniture, for example, raising the height of an armchair, bed, or using a raised toilet seat.
- Changing activities you do to reduce pain.
Only when the above measures fail to give acceptable pain relief, will a Total Hip Replacement be offered to you.
What are the benefits of Hip Surgery?
Once your new joint replacement has healed properly you should look forward to some, or all, of the following benefits.
- Greatly reduced joint pain
- Correction of deformity, for example, unequal leg length.
- Improved quality of life by allowing you to do daily activities in greater comfort.
What to expect after Hip Replacement?
It is important to realise that not all your hip pain may be abolished after your surgery. Immediately after surgery, the gnawing severe pain will have gone and be replaced by surgical pain. This may last up to 6-12 weeks but should lessen over time. Pain medication may still be needed because of this.
You may experience occasional pain in your new hip after walking and other activities. The relief of this type of pain is individual, depending on the severity of any pre-operative deformity in your hip, on the state of your muscles, and so on.
Remember your surgeon replaced only the damaged joint surfaces but could do nothing to the muscles, ligaments and other soft tissues equally damaged by the “joint” disease.
What are the Hip Post Operation complications?
Total hip replacement is successful in nine out of ten people.
As with all major surgical procedures complications can occur, although everything possible is done to minimise the risks. It is important that you understand the following before undertaking your joint replacement surgery.
This is not intended to be a complete list of all the possible complications, but these are the most common:
- Anaesthetic risks - will be discussed with you by your anaesthetist.
- Between 10 - 30 in a 100 chance of Deep vein thrombosis (DVT) - a blood clot in the calf despite preventative measures.
- 1 in a 100 chance of Pulmonary Embolism – blood clot in the lungs.
- A 1 - 3 in a 100 chance of infection. This can occur whilst you are still in hospital. Others may not become apparent for months or even years after the surgery. If your hip replacement gets infected, part or all of it may need to be removed. It is usually possible to have a good result from revision surgery. If this fails it can lead to having the hip replacement removed and replacing it with a scar tissue ‘joint’. This is the way hip osteoarthritis was treated before hip replacement was invented. With a stick and a shoe raise most people would eventually be able to walk comfortably.
- Infection can spread from other areas. Your surgeon may want to make sure that you take antibiotics if you need surgical procedures on your bladder or bowel. It is important to let your dentist know that you have had a joint replacement, as some dental procedures may require you to take antibiotics to reduce the risk of germs spreading to your joint replacement.
- Loosening – This is a major reason replacement joints fail. A loose joint replacement causes pain, and eventually it will need a further operation to revise the joint.
- ·Between 4-8 in a 100 chance of dislocation in the first year. Just like your real hip, an artificial hip can dislocate if the ball comes out of the socket. There is a greater risk in the first 12 weeks after surgery, before the tissues around the hip have fully healed, but there is always a risk. A hip that dislocates frequently may need revision surgery to make it more stable. The physiotherapist will instruct you very carefully how to avoid activities and positions, which may cause the hip to dislocate.
- Damage to nearby blood vessels and nerves is very rare but may sometimes happen.
- Less than 1 in a 100 chance of fractures to the thigh bone. This can occur during surgery.
- You may sometimes find your leg is a little longer or shorter than it was before your operation and a shoe raise may be required.
- 1 in a 100 chance of death. The commonest causes are blood clots on the lungs or heart problems.
Your Hospital Stay
What happens before my admission to hospital?
- You will come to show the reports and meet the Anaesthetist about a week prior to your date of surgery. Usually you will be admitted on the day before your surgery.
- For 72 hours prior to admission, avoid alcoholic drinks, and drink 3-4 litres of fluid, for example, water, tea every day.
- If you smoke, try to stop prior to your admission to hospital.
- If you develop a cough, cold, chest or skin infection, or infected in-growing toenail, please let us know, as it may be necessary to postpone surgery until you have recovered.
What will happen on admission to hospital?
- The anaesthetist will see you after you are admitted. They will discuss the anaesthetic with you and your pain management after the operation. You can discuss any worries you may have.
- If you did not see a doctor at your pre-operative visit, the doctor will see you, explain the operation again, and you will countersign your consent form. You may go for an x-ray if necessary.
- The doctor will also mark your hip for operation with a felt tip pen.
What will happen on the day of my hip operation?
- You will not be able to eat or drink (including water, sweets) for a minimum period 6 hours before your surgery.
- You will be asked to take a bath or a shower before the operation.You will be taken to theatre by a nurse
The Hip Replacement
There are three major types of artificial hip replacement
- Cemented prosthesis.
- Uncemented prosthesis.
- Hybrid prosthesis where one component is cemented in place and the other component is uncemented. A cemented prosthesis is held in place by acrylic cement that attaches the metal to the bone.An uncemented prosthesis has a finish that allows the bone to grow onto the mesh surface and attach the hip replacement to the bone.

Hip Replacement Precautions
There are four basic movements you should avoid for 12 weeks after the operation to minimise the risk of dislocation:
DO NOT bend down to touch below either knee.
DO NOT bring your operated leg up towards your body.
DO NOT cross your legs.
DO NOT twist your new hip.
To avoid bending hip Past 90º (a right angle).
Each hip replacement is made of two main parts:·
- The acetabular component (socket) replaces the acetabulum. There are many types of acetabulum used. Your surgeon will decide which one is the best for you based on your age and lifestyle. The acetabular component can be made of a ferehigh-density polyethylene (very hard wearing plastic).The plastic is so tough and slick you can ice skate on a sheet of it without much damage, or it can be made of metal with either a high-density polyethylene or ceramic liner.
- The femoral component (stem and ball) replaces the femoral head. The femoral component is made of meta, chrome cobalt. The metal stem can be attached to a metal or ceramic ball.
The Operation
The surgeon begins the procedure by making an incision on the side or the back of the thigh to allow access to the hip joint. Several approaches can be used to open up the joint. The choice is usually based on the surgeon's training and preference.
Once the hip joint is visible, the surgeon dislocates the femoral head from the acetabulum. The femoral head is then removed by cutting through the femoral neck with a power saw.
To begin replacing the femur, special rasps (filing tools) are used to shape the inside of the femur to the exact shape of the metal stem of the femoral component. Once the size and shape are satisfactory the stem is inserted into the femoral canal. Again, in the uncemented variety, the stem is held in place by the tightness of the fit to the bone. In the cemented variety, the femoral canal is enlarged to a size slightly larger than the femoral stem and the cement is used to bond the metal stem to the bone. The ball is then attached to the femoral stem. Once the surgeon is happy that everything fits properly, the incision is closed with stitches. Several layers of stitches are used under the skin and either stitches or metal staples are used to close the skin. A sterile dressing is applied to your hip wound.
After the operation you will wake up in the recovery room in your bed. The following may be attached to you:
- An oxygen mask.
- A drip in your arm.
- A blood transfusion may be necessary.
- A catheter - a tube into your bladder.
- Drains to remove excess blood from your wound.
- Pain relief system - remember we can only help you if you tell us how the pain is.
- You may have a pillow between your legs.
Once you have recovered from your anaesthetic you will taken back to the ward where the nursing staff will monitor you regularly. You may feel tired and drowsy, so it is advisable to keep visitors to a minimum.
These precautions are important and will affect how you carry out every day activities. What will happen on the days following my surgery?
Day one
- You will be assisted with a full bed bath.
- You will have a blood test.
- The drip will be taken down if you are drinking well, not feeling sick and do not need a blood transfusion.
- The drains and dressings will be removed.
- You will be able to start some exercise, under the supervision of the physiotherapist. The exercises are shown on page 14. You will be given breathing exercises to help your chest after the anaesthetic, and they also help circulation. Moving both your feet and ankles up and down and in circles quite vigorously also helps circulation.
- If you feel well enough, you will be able to sit out of bed, with assistance. You may feel tired so take it slowly.
- When lying in bed, or sat in the chair, keep moving feet and ankles up and down to help with your circulation.
- The physiotherapist or assistant will see you once or twice a day.
- Use the advice and exercises in this website to help you treat yourself regularly.
- You will start to walk, usually with a walker at first, and gradually progress to crutches.
Day two
- The hip will still be sore, so keep taking pain relief medication as needed.
- Elevating the leg on the bed will also help reduce swelling.
Day three and onwards
- You will have a check x-ray taken when if one has not already been done.
- Your walking will continue to improve as you become more confident.
- The catheter in your bladder, if you have needed one, will be removed when you are able to walk to the toilet, and you will be given an injection of antibiotics.
- When you are safe on your crutches, the physiotherapist will show you the correct way to go up and down stairs (if appropriate).
When can I go home?
You will be allowed to go home when everyone is happy with your progress. You will also need to be safe on your crutches, be able to go up and down stairs, manage to get off a chair, toilet and bed, and generally be able to look after yourself at home if necessary.
Most people leave hospital 5-7 days following their surgery. If there are any post-operative complications, then you may need to stay longer. An ambulance might be the most convenient way to get home..
What should I be doing at home?
Continue with all your exercises and keep progressing your walking. You will need to return to the hospital about 14 days after your operation, to remove stitches or clips from your wound
You will attend the outpatient clinic to see the doctor or nurse 6-12 weeks after your surgery.
Remember, every patient and every joint is different, and that this booklet is only meant as a guide, as to what may happen during your hospital stay. Don’t worry if some days your leg is more stiff, swollen or painful than others, it will get better.
Please seek advice if you experience any of the following
- The wound bleeds or discharges continuously.
- You feel feverish, shivery, have a temperature or feel sick.
- Your wound/leg becomes very hot and red. (It is normal for the wound to feel warm to touch).
- Increased pain not helped by medication or rest.
- Increased painful swelling not helped by ice and elevation
- Increased pain in the calf muscle.
- Sudden onset of shortness of breath and pain when you take a breath in.
Seating/Furniture Heights
You need to be sure that anything you sit on is high enough – your bottom should be at least as high as your knees, and your thighs should slope away from you. You may need a raised toilet seat, and your chair or bed may need to be raised up. Your physiotherapist will advise you on the ideal furniture heights and help to arrange this prior to your discharge.Try to arrange your chair so that telephone, coffee table etc can be reached without twisting.
Sleeping
You will need to sleep on your back for the first 6 weeks. From 6-12 weeks you are allowed to sleep on your operated side when comfortable to do so. After 12 weeks you are able to sleep on either side.
Domestic Activities
You will need some help with shopping, cleaning and laundry.
Cooking
You will still be able to make your meals, but remember, you may feel more tired when you first come home.
You will need to use walking aids, so you won’t be able to carry meals from one room to another.
Social
You may still want to go out – just remember that you will need something suitable to sit on. You may need to take your toilet seat. Try to avoid crowded places where you would be tempted to twist, or be jostled.
Transport
Most people can travel in a car as a passenger after surgery.
To get into and out of the car on the passenger side:
- Park the car away from the kerb, so that you are standing on the same level as the car.
- Have the seat pushed as far back as possible.
- Have the seat reclined.
- Place a cushion on the seat to increase the height of the seat.
- Place a plastic bag on the seat; this will make it easier to swing your legs around.
- Before sitting down, put your left hand onto the top of the passenger seat for support, and with the door window fully wound down, grip the open door window frame with your right hand. Someone should hold the door to prevent you pulling it towards you.
- Gently lower yourself down and remember to keep your operated leg straight out in front of you and do not twist.
- Slide back over the passenger seat until your bottom is well back, use the drivers seat too if necessary.
- Swing both legs around together, remembering to keep your leg in line with the shoulder on the same side.
- Remove the plastic bag before travelling and re-insert the plastic bag when getting out of the car.
- To get out of the car, do the same procedure in reverse.
Physiotherapy Rehabilitation
The following exercises will be taught to you during the first few days of your hospital stay. These exercises will help you to recover more quickly from the surgery. They should be performed 3-4 times a day, 5-10 repetitions of each.
Circulatory exercises – to be performed hourly for the first 1-3 days after your operation.

Bend and straighten your ankles briskly. Repeat ___ times.

Lying on your back or sitting rotate your ankles. Change directions. Repeat ___ times.
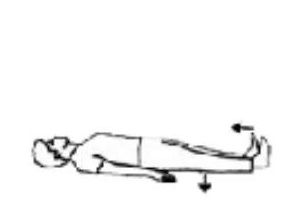
Lying on your back or sitting with legs straight. Pull your toes up towards you and push your knee down firmly against the bed. Hold 5 seconds. Repeat ___ times.
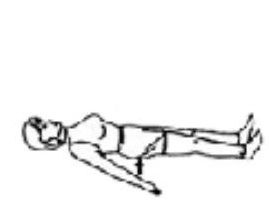
Lying on your back. Squeeze buttocks firmly together. Hold 5 seconds. Repeat ___ times.
The following exercises may be performed, as your discomfort settles and your leg becomes stronger. You should be able to do these exercises whilst you are in hospital, if not, they should be introduced soon after returning home.
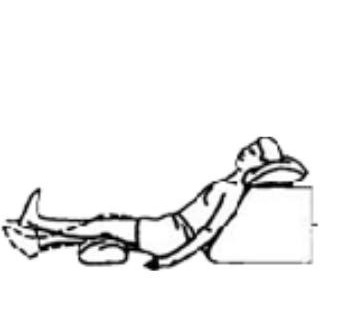
Sitting with back supported. Place a rolled towel under your knee. Pull your toes up towards you, straighten your knee and push it down against the towel. Hold 5 seconds. Repeat ___ times.
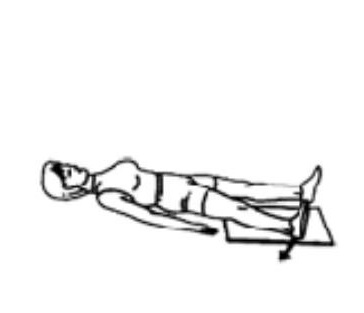
Lying on your back with a sliding board under your leg. Bring your leg to the side and then back to mid position. Please check with your physiotherapist before doing this exercise. Repeat ___ times.
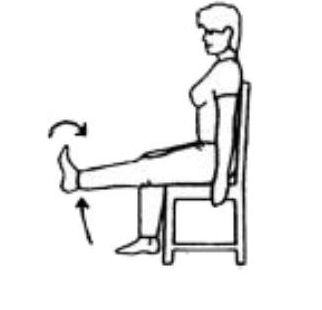
Sit on a chair. Pull your toes towards you, tighten your thigh muscle and straighten your knee. Hold 5 seconds. Repeat ___ times.
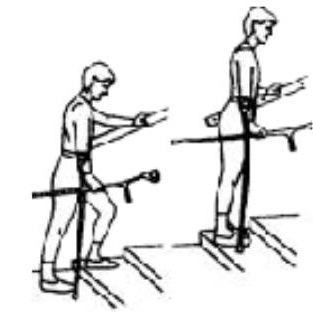
First take a step up with your healthy leg. Then take a step with your affected leg. Then bring your crutch up onto the step. Always go one step at a time.
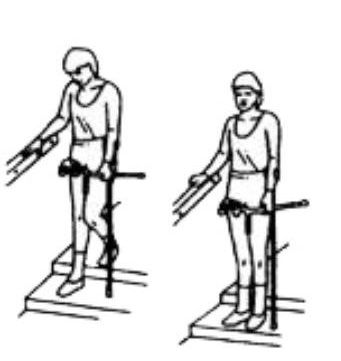
First put your crutch one step down. Then take a step with your affected leg. Then take a step down with your healthy leg, onto the same step as
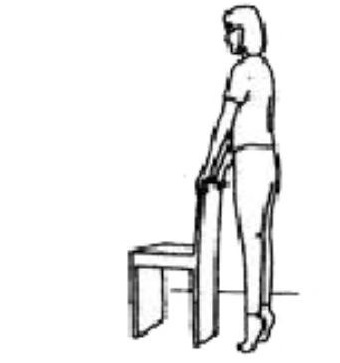
When you are walking well without crutches the following exercises will help you to return to your normal functional activities.
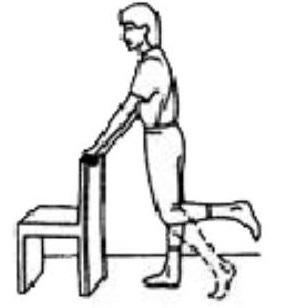
Stand with support. Bend your operated leg behind you and lift your foot off the floor. Repeat ___ times.
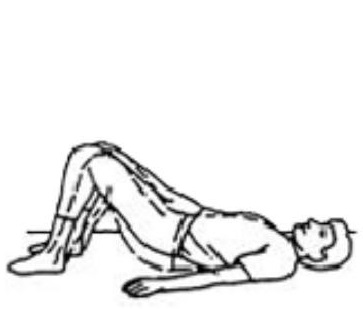
Lying on your back with knees bent. Squeeze your buttocks together and lift your bottom off the floor. Return to starting position. Repeat ___ times.
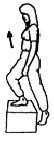
Stand in front of a 20-40 cm step. Step up ___ times with one leg leading and then repeat with the other leg leading. You will need to use the banister. Repeat ___ times.
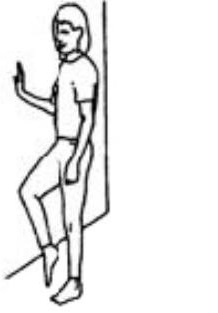
Stand with/witho ut support. Lift one leg and balance.
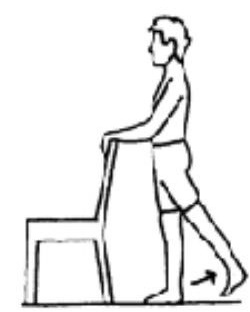
Stand straight holding on to a chair. Bring your leg backwards keeping your knee straight. Do not lean forwards. Repeat ___ times.
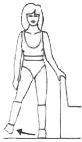
Stand straight holding on to a support. Lift your leg sideways and bring it back keeping your trunk straight throughout the exercise. Repeat ___ times. The nature of your operation will determine if you can perform this exercise, or whether you need to wait 3 months following your operation. Check with the physiotherapist whilst you are on the ward.
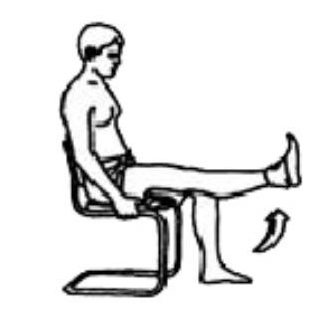
Sit on a chair, with a cushion under your knee and a ___kg weight around your ankle. Pull your toes up towards you, tighten your thigh muscle and straighten your knee. Hold 5 seconds. Repeat ___ times.
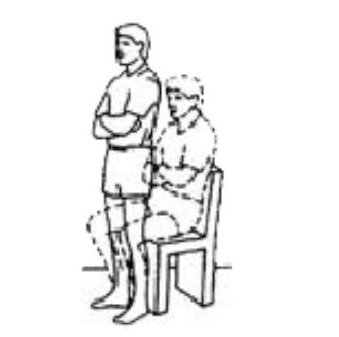
Sitting with your arms crossed. Stand up and then sit down slowly on a chair. (This can be made easier or more difficult by changing the height of the chair). Repeat ___ times.
Skin care
Once the wound has healed, you can massage the scar and surrounding area with a non-perfumed moisturising cream or oil. This helps to keep the skin supple and mobile. If you expose the scar on your leg to the sun make sure you apply a sun block or high factor sun cream to the scar, as initially it is very sensitive and can burn easily.
Remember to let your dentist know that you have had a joint replacement. The dentist may need to give you antibiotics following certain dental procedures to prevent infection.
Commonly Asked Questions
Can I return to playing sports after my total hip replacement?
You can return to playing low-impact sports. This means sports that don’t put high stresses on your hip. These include golf, bowling, cycling or swimming
When will I experience the full benefit from hip surgery?
Although you will experience relief of your pre-operative pain quite soon after the operation, the return of full function can take much longer. After three months, you will probably have regained some of the strength in the muscles in your leg, and range of movement will be improving. However, it may take up to 18 months to feel the full benefits.
How long will the joint replacement last?
The lifetime of the joint replacement varies from person to person. It can depend on many factors such as the patient’s activity level, body weight and surgical technique. A replacement joint is not as strong or durable as a natural healthy joint. There is no guarantee that a replacement joint will last the rest of a patient’s life.
When will I be able to drive?
Do not drive until you can safely do so (please check with your insurance company).
You are able to drive 6-12 weeks after the operation, providing there have been no problems in your rehabilitation.
When will I be able to fly?
You are able to fly no sooner than 6 weeks after your operation. Your risk of having a DVT (blood clot in the calf) is still high within this time period.
Will I set off the alarm at the airport?
The joint replacement is made of cobalt chrome and, in theory, shouldn’t set off the alarms. If the alarm does go off, then the scar on your thigh will help confirm that you have had surgery. If you are worried then you could ask your consultant for a letter to confirm you have had a joint replacement.
Will I be pain free?
The majority of patients may well be pain free and no longer need painkillers. About a third of patients will have some pain, but it should be much less than the pain they had before the operation.
What about sex?
Generally, patients resume sexual activities as soon as they feel able, usually from 6 weeks onwards. In the months following surgery, patients are generally advised to take it easy and modify their positioning to keep pressure off the affected joint whilst it is healing.
Do’s
- Keep active when you are on the ward. It will be much easier to walk around with crutches at home rather than a frame.
- Gradually increase the distances walked at home, as pain allows.
Don’ts
- Bend the hip beyond 90º (a right angle) for the first 3 months.
- Cross your legs, as this is a risk position for hip dislocation.
- Twist and turn on your operated leg. Make sure you lift your feet when turning.
- Sit on a low chair, bed or toilet.
When you get home
Please remember that you have had a major operation and your recovery will be gradual.
Swelling
Swelling is a normal reaction after your surgery and aids the healing process. As you have had major surgery the swelling can initially be quite severe.
The swelling should follow a daily pattern whereby it gets better while you are sleeping and may get worse during the day. As long as the swelling gets better while you are asleep then this is normal.
If the swelling gets worse overnight, becomes hard, shiny and painful, you should contact the hospital or your GP.
Walking
You will be taught the correct way of walking with the appropriate walking aids and loaned the necessary aids to take home. This will depend on the type of operation and which consultant performed the surgery. You should comply with the instructions given in hospital.
It is important to get yourself up and about regularly throughout the day. General advice is that you get up and have a walk at least once every hour.
Your body will only be used to doing the same amount of exercise as you were doing before the operation an d then you will get tired. As you continue to mobilise you will find you can get further before you tire. You can walk outdoors when you feel confident enough.
